Making sense of all those Medicare Enrollment Periods can be daunting . You are not alone! We will explain each of them in a straightforward and easy to understand manner.

Enrollment Periods
– The Medicare Initial Enrollment Period (IEP) –
During the Medicare Initial Enrollment Period, individuals have a 7-month window to enroll in Parts A and B for the first time when they reach the age of 65. The enrollment period includes 3 months prior to turning 65, the month of turning 65, and 3 months after. However, if enrollment occurs during the 3 months after the 65th birth month, coverage will be delayed. This 7-month window also allows for enrollment in a Medicare Advantage or Part D plan.
– Annual Election Period (AEP) –
The Annual Election Period (AEP) commences on October 15th and concludes on December 7th annually. During this election period, Medicare beneficiaries who already possess Part A and Part B have the opportunity to enroll in, modify, or discontinue their Part D or Medicare Advantage plan.
– General Enrollment Period ( GEP) –
The General Enrollment Period is used to enroll in Medicare Part A and/or Part B if you missed your IEP and do not qualify for a Special Enrollment Period. The GEP window starts January 1st and ends March 31st of each year and coverage will begin the 1st of the month after you apply.
– Medicare Advantage Open Enrollment ( MAOEP ) –
This enrollment period is specifically designed for beneficiaries who are currently enrolled in a Medicare Advantage plan but wish to discontinue it. Within the MAOEP window, which spans from January 1st to March 31st, you have the opportunity to transition from your existing Advantage plan to a different one or opt for Original Medicare along with a Part D plan.
– Special Enrollment Period (SEP) –
A beneficiary can utilize a Special Enrollment Period whenever they experience a qualifying event. In the event that you postponed enrolling in Medicare after turning 65 because of having creditable coverage through active employment, you can take advantage of this enrollment period to apply for Medicare A and B. Additionally, there are Special Election Periods (SEP) available for Medicare Advantage and Part D plans. If you encounter a qualifying event, you will be given a 2-month time frame to enroll in either a Medicare Advantage plan or Part D plan.
– Supplemental Medigap Open Enrollment Period –
Upon initial enrollment in Medicare Part B, individuals are granted a 6-month period before and after their Part B effective date to enroll in a Medigap plan without the need to answer any health-related inquiries. However, if one misses this window and lacks a qualifying event, they may be required to respond to health questions in order to enroll in a Medigap plan.
Medicare Statistics
According to a report released in 2012 by the Medicare Rights Center, approximately 700,000 individuals faced a late enrollment penalty for Part B during that year. It appears to be quite common for people to miss their Medicare enrollment period. The situation is further complicated by the existence of various enrollment periods, such as the Medicare Initial Enrollment Period, the Medicare Supplement (Medigap) Open Enrollment Period, the Medicare Annual Election Period, and the Medicare Special Enrollment Periods.
It’s no wonder that it can be overwhelming to keep track of all these different periods!
Furthermore, around 12% of Medicare beneficiaries did not have creditable prescription drug coverage, which means they could potentially face a premium penalty when they eventually enroll in a Part D Drug Plan.
This means that approximately 6 million individuals could end up paying monthly penalties for as long as they have Medicare coverage. Over the years, this could amount to a significant sum of money.
To avoid finding yourself without essential healthcare coverage or paying more than necessary for the coverage you desire, it is crucial to familiarize yourself with the various Medicare enrollment periods for 2024 and beyond.
Medicare Initial Enrollment Period
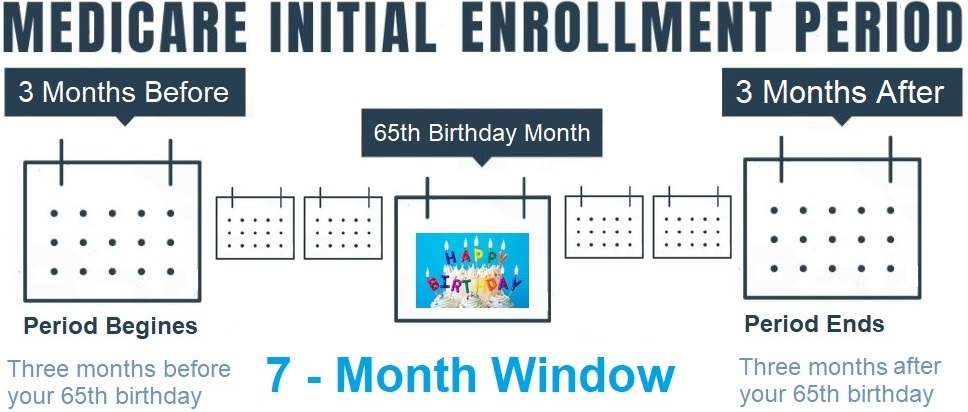
The Medicare Initial Enrollment Period holds significant importance as you near the age of Medicare eligibility. This seven-month period, known as the Initial Enrollment Period (IEP), commences three months prior to your 65th birthday, encompasses your birthday month, and continues for three months after.
During your Medicare Initial Enrollment Period (IEP), you have the opportunity to enroll in Original Medicare (Part A and Part B) or a Medicare Advantage plan (Part C). This period typically lasts from February 1st to August 31st, but if your birthday falls on the 1st of the month, your IEP will start one month earlier. For instance, if your birthday is on April 1st, your IEP will begin on December 1st, and your Medicare coverage will start on March 1st.
Enrolling in Medicare during your IEP is crucial as it helps you avoid any late enrollment penalties. Additionally, if you require prescription drug coverage, you can enroll in a Part D plan during this same window. This drug coverage can either be a standalone plan or part of a Medicare Advantage plan that includes Part D.
If you choose Original Medicare, you may also consider obtaining additional coverage through a Medicare Supplement Plan (Medigap). To do so, you can utilize your Medicare Supplement Open Enrollment Period (OEP), which is a 6-month window starting on your Part B effective date. The advantage of using the Medigap OEP is that you cannot be denied coverage for any Medigap plan available in your area, regardless of your health status. Furthermore, your insurance company cannot charge you higher premiums based on your health status or pre-existing conditions, and your coverage for any pre-existing conditions cannot be delayed.
What happens if I miss my Initial Medicare Enrollment Period?
 If you choose not to enroll in coverage during your IEP and do not have any other creditable coverage, such as employer coverage, there are several negative outcomes that you may encounter.
If you choose not to enroll in coverage during your IEP and do not have any other creditable coverage, such as employer coverage, there are several negative outcomes that you may encounter.
If you fail to enroll in Part B during your Initial Enrollment Period (IEP), you will most likely be subject to a late enrollment penalty that will continue for the duration of your Medicare coverage. The penalty amounts to 10% for each 12-month period that you were eligible for Part B but did not enroll. As of 2024, the standard premium for Part B is $174.70, resulting in an additional monthly payment of $17.01. It is important to note that this penalty may increase if the standard Part B premium rises in the upcoming year, which is highly probable. Even if you ultimately decide to opt for Medicare Advantage, you will still be required to pay this penalty. You have the option to forgo Part B coverage for a substantial period of time. If you do not enroll during your IEP, you will need to wait until the next General Enrollment Period, or GEP. Your coverage will not commence until the first day of the following month after your application is submitted.
If you fail to have credible Part D prescription drug coverage and miss your IEP, you will be subject to a penalty on your Part D premium. This penalty amounts to 1% for each consecutive month that you went without coverage for prescription drugs. Currently, the national base premium is approximately $34.70 per month. Therefore, if you go without coverage for a year, you will be required to pay an additional $3.96 per month (and potentially more if the Part D base premium increases) for as long as you maintain coverage.
If you find yourself in the uncommon scenario where you are ineligible for premium-free Part A due to insufficient work credits and you fail to purchase it during your IEP, you will incur a 10% premium penalty for double the number of years you could have obtained the coverage but chose not to.
If I miss my IEP, when will I be eligible for Medicare Advantage or Medicare Part D?
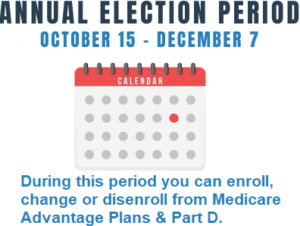 The Annual Election Period (AEP) takes place from October 15 to December 7 every year and is specifically designed for Medicare Part C and Part D, which includes Medicare Advantage plans and prescription drug plans. If you happen to miss your initial Medicare enrollment period, you can utilize the next AEP to join a plan. During the AEP, you have the option to switch from Original Medicare to Medicare Advantage. If you are already enrolled in a Medicare Advantage plan, you can also change to a different one. In case you decide to join a Medicare Advantage plan but later wish to return to Original Medicare, the AEP allows you to do so. Additionally, you can enroll in a Medicare Part D prescription drug plan during the AEP, or switch to a different plan if you are already enrolled. If you have obtained creditable coverage through an employer or another source, you even have the flexibility to completely drop your Part D coverage without facing any penalties.
The Annual Election Period (AEP) takes place from October 15 to December 7 every year and is specifically designed for Medicare Part C and Part D, which includes Medicare Advantage plans and prescription drug plans. If you happen to miss your initial Medicare enrollment period, you can utilize the next AEP to join a plan. During the AEP, you have the option to switch from Original Medicare to Medicare Advantage. If you are already enrolled in a Medicare Advantage plan, you can also change to a different one. In case you decide to join a Medicare Advantage plan but later wish to return to Original Medicare, the AEP allows you to do so. Additionally, you can enroll in a Medicare Part D prescription drug plan during the AEP, or switch to a different plan if you are already enrolled. If you have obtained creditable coverage through an employer or another source, you even have the flexibility to completely drop your Part D coverage without facing any penalties.
When is the Medicare General Enrollment Period?
If you have missed your IEP and do not qualify for a special enrollment period, you have the option to enroll in Original Medicare during the General Enrollment Period (GEP). The GEP takes place from January 1 to March 31 each year, and your Medicare Part B coverage will become effective on the first day of the following month after you submit your application.
However, it is important not to mistake the GEP as a safety net that exempts you from worrying about your IEP. Even though you can sign up for Original Medicare during this period, you may still be subject to late enrollment penalties.
Please note that the General Enrollment Period only applies to Original Medicare. If you are interested in a Medicare Advantage plan or Medicare Part D coverage for prescription drugs, you will need to wait for the Annual Enrollment Period.
What happens if you don’t enroll in Medicare Part A at 65?
If you have creditable coverage beyond the age of 65, you will be eligible for a Special Enrollment Period to apply for Medicare once your coverage ends. However, if you do not have creditable coverage, you will have to wait until the General Enrollment Period to apply. Moreover, if you start receiving Social Security benefits after turning 65, you will be enrolled in Part A automatically if you are not already enrolled. As long as you meet the requirements for premium-free Part A, you will not face any penalties for enrolling in Part A.
The Medicare Advantage Open Enrollment Period
The Medicare program offers an opportunity for you to reconsider your decision regarding a Medicare Advantage plan. If you have enrolled in a Medicare Advantage plan and find that it doesn’t meet your needs, you have the option to disenroll during the Medicare Open Enrollment Period, which takes place from January 1 to March 31. During this period, you can choose to return to Original Medicare and also select a Part D drug plan to complement it. Additionally, you have the option to switch to a different Medicare Advantage plan once. However, it’s important to note that if you decide to return to Original Medicare and are considering getting a Medigap plan, there is no guarantee of acceptance. In many cases, you may be required to answer health-related questions for the Medigap plan, and the insurance carrier has the discretion to accept or reject your application.
Medicare Special Enrollment Period
The Medicare Special Enrollment Period (SEP) is an eight-month timeframe that commences either when you or your spouse ceases employment or when your group coverage terminates, whichever occurs first. Specific circumstances unique to you can trigger a Special Election Period (SEP) for a Part D or Medicare Advantage plan.
Typically, a Medicare Special Election Period lasts for two months and allows you to modify your coverage due to a special circumstance. For instance, if you relocate outside the plan’s service area, you will qualify for a Special Election Period.
During the SEP, you have the option to switch to a new Medicare Advantage or Part D prescription drug plan. Additionally, you can return to Original Medicare without facing any penalties. In some cases, you may also be able to enroll in Medigap under guaranteed issue rights, which means there will be no medical underwriting. However, please note that this rule may vary depending on the state you reside in.
There are also other situations in which you may be eligible for a Special Election Period. If your specific circumstance is not mentioned above, please contact us to explore the options available to you.
Creditable Coverage
In many cases, individuals continue to maintain group coverage through their employer or union plan, enabling them to postpone their enrollment in Part A and/or B. Upon retirement, they can avail themselves of a Special Enrollment Period to enroll in these Parts. Medicare acknowledges and credits individuals who possess employer group coverage from any sizable employer with 20 or more employees.
Medigap Open Enrollment Period
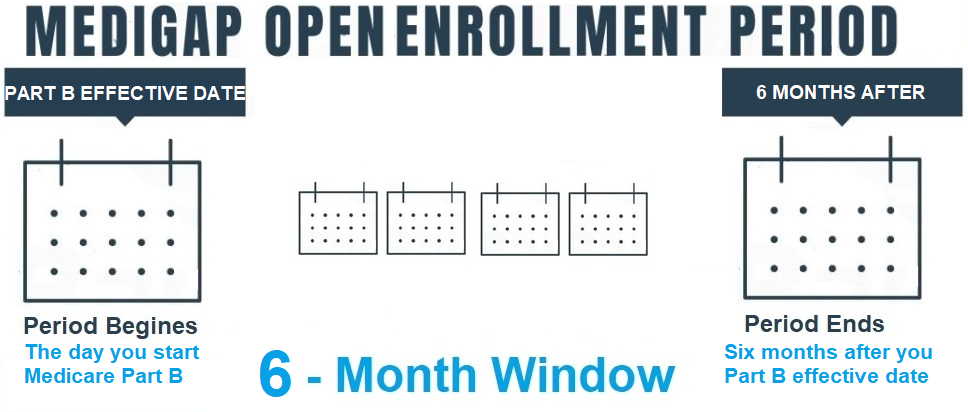
It is crucial to understand that this enrollment period occurs only once for the majority of individuals. Once it passes, it will never return, making it one of the Medicare enrollment periods that must not be overlooked.
Get Help with Your Medicare
You have earned your Medicare benefits through your hard work, now its time to ensure that you have full healthcare coverage. However, it is crucial to familiarize yourself with the rules, regulations, and your rights and benefits under Medicare insurance. To ensure that you receive all the benefits available to you under the Medicare program, it is important to understand the key enrollment periods.
Missing an important date could have long-term consequences for you. If you want to avoid any Medicare late penalties and ensure that you don’t miss any deadlines, reach out to Cindy’s Health Insurance Services today. Our team will assist you in determining when to enroll, so you can stay on top of your Medicare coverage.
Takeaways
Medicare offers distinct enrollment periods, designated time frames that enable individuals to submit their applications for Medicare coverage. There exist three enrollment periods specifically for enrolling in Medicare Parts A and B. Additionally, Medicare Advantage plans, Part D plans, and Medigap plans each have their own unique enrollment periods, allowing individuals to enroll, disenroll, or switch plans throughout the year.
 Mario Arce
Mario Arce
I have been working with Medicare clients since 2016. I serve California members in San Bernardino & Riverside county.

