As you may be aware, Medicare, the federal government health insurance program in the United States, does not provide coverage for all medical expenses. To fill in the gaps, many individuals opt to purchase additional insurance. When comparing Medigap and Medicare Advantage, it is crucial to understand that both types of Medicare plans can assist in reducing your out-of-pocket expenses. After all, who wants to face a deductible of $1,632 or more every time they are admitted to the hospital? Or be responsible for paying 20% of the cost of a costly MRI? Therefore, the two primary coverage options available to help with these expenses are Medicare Advantage and Medigap (also known as Medicare Supplement). It is essential to have a clear understanding of how each type of coverage functions so that you can choose the most suitable plan for your needs.

Comparing Medicare Advantage and Medigap (Medicare Supplement): Selecting the Superior Option.
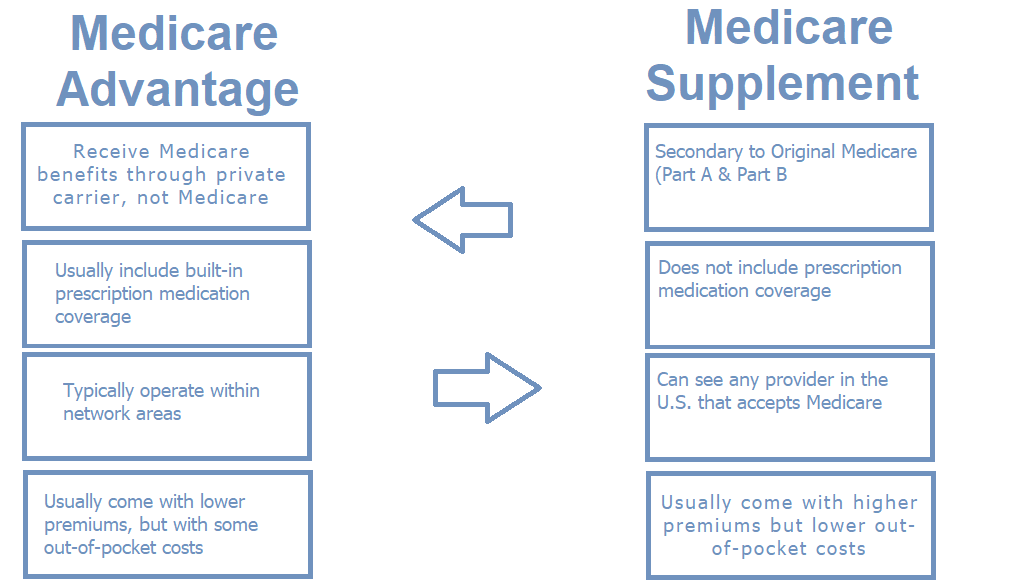
Medicare supplements and Medicare Advantage plans, serve the purpose of covering the gaps in Medicare. However, they have distinct designs and functions. Medicare supplements act as secondary insurance to Medicare Part A and Part B. In this setup, Medicare pays its portion of the bill first, and then the remaining balance is sent to your supplemental company. Depending on the plan you are enrolled in, the supplement company will pay its share accordingly. Each Medigap plan offers different benefits, with Plan F, Plan G, and Plan N being the most popular choices.
On the other hand, Medicare Advantage plans are completely separate from Medicare. When you opt for a Medicare Advantage policy, you receive your benefits directly from the plan itself, rather than from Medicare. By enrolling in this type of plan, you agree to utilize the plan’s network of healthcare providers, except in cases of emergency care. As you receive healthcare treatment, you will be responsible for paying copayments along the way. These plans can be seen as an alternative to Original Medicare.
Medicare Supplement Plans: An Overview
Medicare supplement plans, also known as Medigap plans, provide additional coverage to individuals who are enrolled in Original Medicare. Unlike HMO Advantage plans, Medigap plans allow you to choose any provider that participates in Medicare, regardless of the supplement company you select. With a Medigap plan, you are not required to choose a primary care doctor, and you have access to all Medicare providers nationwide without the need for referrals.
By enrolling in a comprehensive plan such as Plan F or Plan G, you can significantly reduce your out-of-pocket expenses. This means that you won’t have to worry about paying for doctor copays or coinsurance. Just like Original Medicare, Medicare Supplement plans cover medically necessary doctor visits, specialist care, office visits, surgery, procedures, and exams.
When you enroll in a Medicare supplement plan, your insurance company will inform Medicare about your policy purchase. As a result, when Medicare pays its portion of your medical bills, the remaining balance will be automatically sent to your Medicare Supplement insurer. This process is seamless and eliminates the need for you to file any claim forms.
Open Access & Referral-Free.
Medicare Supplement insurance plans provide unparalleled access to healthcare providers, granting you the utmost freedom. With over 900,000 Medicare providers nationwide, you have the liberty to select your preferred doctors and hospitals. Moreover, there is no requirement for referrals when seeking specialized care under this coverage.

The premiums for Medicare Advantage plans are lower compared to these plans, as they provide less freedom and flexibility. Moreover, certain Medigap policies offer coverage for emergency medical services during foreign travel when policyholders are abroad. Insurers will bear 80% of the expenses for such services after the policyholder fulfills the $250 deductible.
Your Part D Drug Coverage is Separate
Medigap plans provide coverage for medications that are administered in a hospital environment, including injectables and chemotherapy drugs. However, it’s important to note that these plans do not cover retail medications. To ensure comprehensive prescription drug coverage, most beneficiaries opt to enroll in a separate Medicare Part D plan. These Part D plans are accessible in all states and typically start at a monthly cost of approximately $10. It is crucial to enroll in a Part D plan and maintain creditable coverage to avoid incurring a late enrollment penalty in the future.
Medigap Enrollments
During your one-time open enrollment window, which occurs within 6 months of your Part B effective date, enrolling in a Medigap plan does not require you to answer any health questions. Your application will be approved by the insurance company. It is worth noting that a majority of Medigap enrollees choose to enroll in a Medigap plan during this specific window.
Furthermore, there are no waiting periods or exclusions for pre-existing conditions when you apply within this enrollment window. However, if you happen to miss this window and apply at a later time, you will typically be asked to answer a series of medical questions and undergo underwriting. It is important to understand that underwriting rules may vary depending on the carrier and state. The underwriter at the insurance company will evaluate your medical history and make a decision to either accept or decline your application.
About Medicare Advantage Part (C)
Approximately 44% of beneficiaries opt for Medicare Advantage policies, which are private insurance plans. These plans generally have lower premiums compared to Medigap plans, and in some cases, they even offer a $0 premium in certain areas. Medicare Advantage programs come in various forms, including HMOs, PPOs, PFFS (private-fee-for-service), and SNPs (Special Needs Plans).
When a plan has a $0 premium, it means that you won’t have to pay any additional premiums for the plan itself. However, you will still need to pay your monthly Part B premiums. To be eligible for a Medicare Advantage plan, a beneficiary must be enrolled in both Medicare Part A and Medicare Part B. Most Advantage plans already include prescription drug benefits, so there’s no need to enroll in a separate Part D plan.
Why would a company offer a $0 premium plan? The reason is that you agree to utilize the plan’s network providers for your healthcare needs. This means you’ll have a more limited choice of doctors compared to choosing a Medigap plan. The insurance company has greater control over the providers and facilities they negotiate contracted rates with.
Before making any decisions, it is crucial to consult your doctors and confirm if they are part of the plan’s network, along with your preferred hospital facility. This becomes even more significant if you are considering an HMO (health maintenance organization) plan, as they typically have smaller networks. In some cases, HMOs may have networks as small as 250 doctors, which is quite limited. Therefore, it is essential to thoroughly research and ensure that physicians in your area accept your plan. Additionally, it is worth noting that PPOs may provide a wider range of options, but your cost-sharing is likely to be higher.
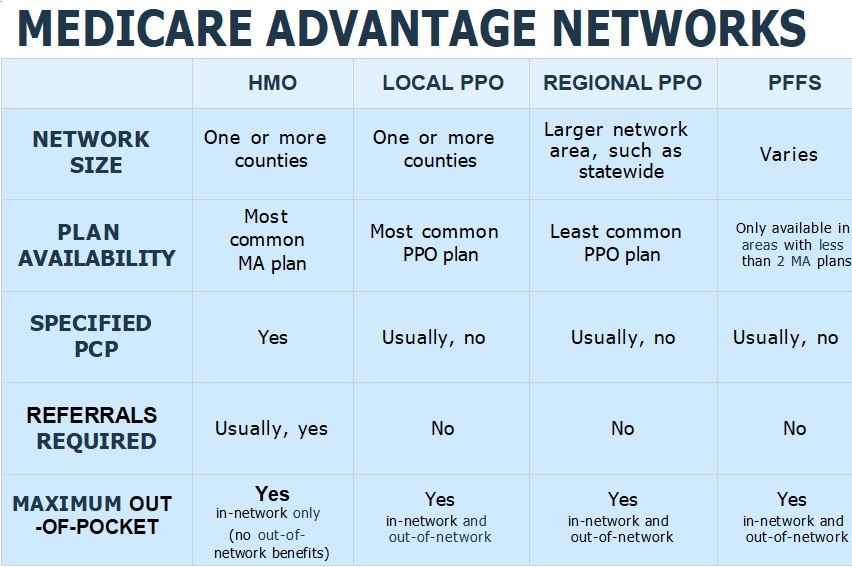
Look for a Medicare Advantage plan that has a wide network of providers in your service area. According to the Kaiser Family Foundation, the average Medicare beneficiary has access to more than 30 Advantage plans in their zip code. With a Medicare Advantage plan, your healthcare bills will be paid by your insurance company instead of Medicare. As you receive services from providers within the plan’s network, you will be responsible for paying copays. It is important to review the copays before enrolling to ensure they are reasonable for you. Additionally, the plan may have certain restrictions on services, such as requiring prior authorization, so it is important to fully understand your benefits.
Keep in mind that copays can vary between different plans. For example, one plan may charge $40 for a specialist visit while another charges $50. It is important to consider your medical usage when selecting a plan, as copays can add up over time. Furthermore, Advantage plans can offer coverage for benefits that Original Medicare does not cover. These may include routine dental, vision, and hearing services, transportation, gym memberships, telehealth services, and even over-the-counter items. Some plans may also provide coverage for hearing aids.
When applying for a Medicare Advantage plan, there are no health questions to answer. However, there are specific enrollment periods throughout the year for enrolling, dis-enrolling, or changing your Advantage plan.
Review the Drug Formulary.
It is worth noting that many Medicare Advantage plans provide Part D coverage, eliminating the need for a separate drug plan. This convenience is appreciated by some individuals. Nevertheless, over the years, I have witnessed a few unfortunate cases where people neglected to verify if their plan covered their required prescription drugs. While they diligently checked with their doctors, they failed to confirm whether their medications were included in the built-in prescription coverage. Consequently, they discovered themselves trapped in a plan that did not offer crucial and often costly medications.

Medicare Advantage plans operate under distinct enrollment periods, including the Medicare Advantage Open Enrollment. Once you enroll in a plan, Medicare binds you to that particular plan until December 31st. However, there is a possibility to switch plans during the year if certain circumstances grant you a special election period, such as relocating to a different state. Hence, it is crucial to exercise prudence when selecting a plan. It is important to remember that in order to qualify for Medicare Advantage, you must be enrolled in both Medicare Parts A and B. It is crucial to note that enrolling in Medicare Advantage does not exempt you from paying the premiums for Part B that you are already responsible for. You will still be required to pay for Part B coverage.
About the Out-of-Pocket Maximum
All Medicare Advantage policies include an Out-of-Pocket (OOP) Maximum Cap, which serves as a safeguard to limit your expenses throughout the year. Starting from 2024, Medicare has set a maximum limit of $8,850 for this cap. However, it is important to acknowledge that $8,850 can be a substantial amount for individuals with fixed incomes. While there may be several years where you won’t come close to reaching this limit, it is crucial to consider the possibility of facing a severe illness, such as cancer, which could quickly lead to reaching the maximum cap. Fortunately, many Medicare Advantage plans offer OOP maximums that are lower than the $8,850 threshold.
Changing Between Medicare Advantage & Supplement Plans
Starting with Medicare Advantage and then transitioning to Medigap coverage may seem like an appealing option – opting for the most affordable insurance until the need arises, and then switching back to a more comprehensive plan.
However, it is crucial to understand that this approach does not work in practice. If you decide to leave a Medigap plan in favor of Medicare Advantage coverage, there is a possibility that you may not be able to return to a Medigap plan later on.
By that time, you may have exceeded your one-time open enrollment window, which means that Medigap insurance companies can inquire about your health status when you apply. They have the authority to reject your application based on specific health conditions or even the medications you take. Therefore, it is essential to consider these factors before making the decision to switch to Medicare Advantage. However, there are certain circumstances that you should be aware of before becoming eligible for Medicare.
Trial Exception
Individuals who are new to Medicare Advantage are eligible for a trial period. In the event that you choose to discontinue your enrollment in the plan and switch back to Original Medicare within the initial 12 months of having Medicare Advantage coverage, you can return to your Medigap plan without undergoing any underwriting process. However, once the 12-month period has elapsed, you will be required to undergo underwriting.
Under 65 Exception
People under the age of 65 who received Medicare early due to a disability are an exception to the rule. While anyone eligible for Medicare can enroll in an Advantage plan, not all Medigap plans are available to those under 65 in many states. This is because Federal law does not require Medigap coverage for individuals under 65. However, certain states such as Colorado, California, Maine, Minnesota, Wisconsin, Oregon, and Missouri offer all Medigap plans to those who qualify for Medicare due to specific disabilities. Once the individual turns 65 and becomes eligible for Medicare based on age rather than disability, they will have a second open enrollment window. During this time, they can switch from Medicare Advantage to Medicare Supplement without undergoing underwriting.
Takeaways
Medicare Supplement and Advantage plans exhibit notable distinctions, with Supplement plans serving as secondary plans while Advantage plans act as replacements for Original Medicare. These plans are provided by insurance carriers rather than the federal government, thereby offering a wide array of choices. However, it is important to note that switching between the two can only be done during specific periods of the year or under specific circumstances.
 Mario Arce
Mario Arce
I have been working with Medicare clients since 2016. I serve California members in San Bernardino & Riverside county.

